Movember: Prostate and Testicular Cancer

It’s November and one of the many events happening this month is the series of fund-raising projects sponsored by the Movember organization highlighting men’s health issues.
The Movember organization began in 2003 to focus on 4 specific men’s health topics: prostate and testicular cancer research and prevention, physical inactivity, and men’s mental health awareness including suicide prevention. To date, they have raised over $837 million for men’s health, funding 1200+ projects in over 20 countries.
Throughout the entire month of November, Movember encourages men to grow out their mustache, walk or run 60 miles throughout the month, and/or sponsor a social event to raise awareness and funds for men’s health. The fundraiser proceeds are donated to men’s health projects, such as TrueNTH (helps men with prostate cancer), TrueNTH Testicular Cancer (provides support for men with testicular cancer) and GAP (international research initiative to tackle prostate and testicular cancer). They are also closely associated with the “Distinguished Gentleman’s Ride” (A vintage motorcycle ride held in various locations around the world to highlight men’s health issues and raise funds).
In today’s post, I want to tackle two of the issues key issues – testicular and prostate cancer. Both cancers are very common in men and merit discussion as to how to prevent and treat them. We will tackle men’s specific mental health and suicide prevention in a later blog post.
Prostate Cancer
Prostate cancer is a very common cause of cancer mortality in men, ranked 3rd behind skin and lung cancer. Currently it is the most common visceral (soft internal organs) cancer diagnosed and is the third leading cause of cancer death in men. Fortunately, a good screening test is now available in the form of the PSA test. (The PSA test is a blood test that measures the amount of prostate-specific antigen (PSA) in the blood. You can read more about the test here.
Unfortunately, there has been recent controversy that makes this issue very confusing for men. Many advisory bodies now recommend against the routine screening of prostate cancer without a discussion about the risk of over diagnosis leading to unnecessary aggressive treatment. The problem is that prostate cancer can remain in a relatively benign (harmless) state and not cause significant problems in a person for many years. On the other hand, aggressively treating the benign cancer with surgery and radiation may result in unnecessary risk and danger.
The recommendation I make to my patients is based on an individual discussion of the risks and benefits of PSA screening. Generally,…
- Men 50 years and older are considered “regular risk” and should strongly consider PSA testing every 1-2 years.
- Men with the following factors are considered “high risk” and should begin PSA screening sooner, between 40-45 years old:
- African-American race
- History of a first-degree relative having prostate cancer at an age less than 65
- Known genetic mutations such as BRAC
Testicular Cancer
When talking about testicular cancer, things are much clearer.
While testicular cancer is much more common in younger men between ages of 20 and 34, the good news is that it is one of the most curable solid neoplasms (new abnormal tissue growth).
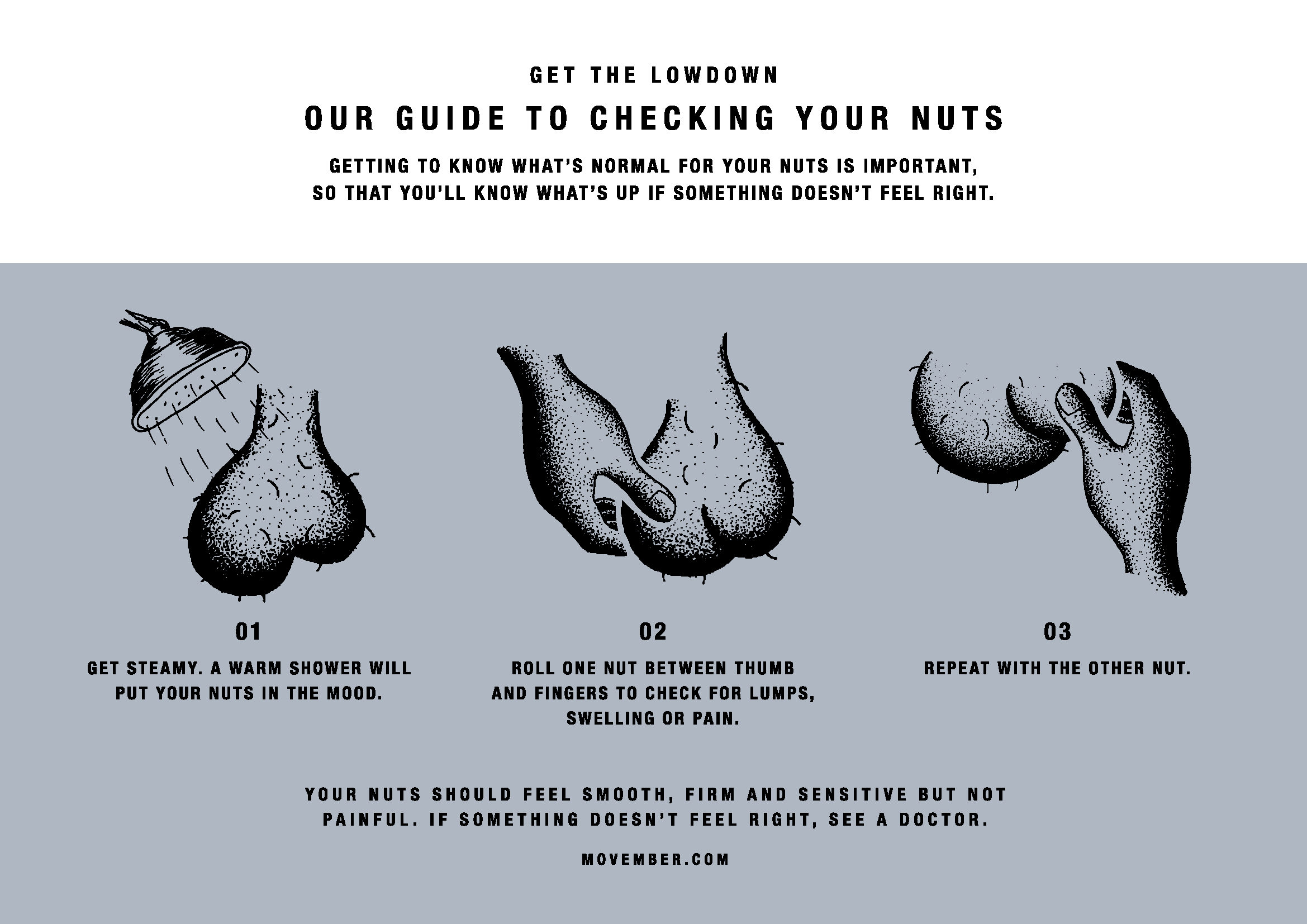
There is no specific recommendation for screening test or routine testicular examination by physicians, unlike the prostate guidelines. However, men should practice monthly routine self-examination at home to monitor for any unusual lumps or tenderness. To learn how to do a self-exam, see below. (You can also download the guide here and watch a video regarding the importance here.)
It’s important to be aware of the key signs to look for and whether you have a medical history that places you at high risk. Risk factors include:
- Undescended testicle
- Family history of testicular cancer
- HIV infection
- Prior history of cancer in one of testicles
- African-American and Asian-American race
It is always tempting to put off routine healthcare maintenance and cancer screening, particularly for men. But men are dying an average of 6 years younger than women and many of the reasons are preventable. Don’t let the complexities and frequent changes in recommendations cause you to put off getting the care you need. If you have any questions concerning your cancer risk or general health, this would be a great time to make an appointment with your primary care team.
In health,
Dr. Bruce Baker
Medical Director
To read more blog posts written by Dr. Baker, click here.